In today’s post, I reveal the 5 types of doctors that hate call the most. How did I conclude this, and how does this correlate with burnout? Read below to find out!

One of the worst aspects of being a physician or health care professional is having to be “on call.” For my non-medical professionals out there, this means that for a set period of time, you’re constantly available for medical emergencies.
I’m a urologic surgeon, so I technically take “home call.” This means that when I’m on home call, if I’m not in the hospital seeing a consult or operating, I could theoretically be at home. Home call is an invention for specialties that typically don’t have as many emergencies that need their immediate presence, like urology or ophthalmology.
“In-house call,” on the other hand, is for specialties where the frequency and acuity of need is typically greater. Examples of these specialties include critical care and general surgery. If someone is having worsening chest pain or a perforating appendicitis, it’s ideal to have these specialists in-house. So these doctors are typically in the hospital when they’re on call, and they sleep in call rooms overnight.
Physicians who take in-house call usually get the next day off to recover. But for those of us who take home call, we tend to work the next day.
There are plenty of types of doctors that hate call, no matter the type. But I take home call, so I’d like to tell you why I find it so horrible.
The problem with “home call”
What happens when you take a “home call” specialist and ask them to take care of about 600,000 lives simultaneously? Even with a statistically lower chance of emergencies, with that many lives there are bound to be plenty of urgent issues.
That leads to a call experience like mine this past weekend, where I spent Saturday working like a maniac for 14 hours straight during the day, plus another two hours from 2-4AM on Sunday morning.
In what I’d consider a moderately bad call day, I fielded about 30 pages, saw five emergency room consults, and did four emergency surgeries. This work was evenly split between two hospitals that are 20 miles apart, so I drove over a hundred miles while juggling the emergencies.
The volume of work was such that I decided to spend the night in the hospital anyway, rather than drive home and risk getting called back again to the hospital.
If this had been a weekday, I’d have had to see patients the next day or operate. Instead, I spent my Sunday in a bleary haze. I remember snapping at my kids and staring blankly at my wife as we went about our weekend routine.
Call was worse during residency training
I still remember my call from residency training with dread. My current overnight calls are easy compared to the 24 hour call days as a resident at LA County hospital. On many of those days, I’d be lucky to have time to use the restroom or eat a meal. I remember getting hammer paged by nurses with mundane requests for tylenol, stool softener, benadryl, etc, etc… This was prior to electronic medical records. So for the first part of my training, I’d have to shuffle to the actual patient chart by their bed. As I wrote, I’d pray that my writing was legible enough so that the nurse could read it the first time. Otherwise, I’d get another page from the nurse, asking for clarification.
It was a teaching hospital, so many of the phone calls were from other residents or medical students, who were just as exhausted and overworked as I was. In residency, all doctors hate call.
During those tough years, I dreamt of the future when I’d be an attending. I imagined my own clinical practice with a tidy waiting room of grateful patients with simple medical issues. Busy call days and nights certainly never entered this fantasy. Instead, I dreamt that my private practice would be supported by referrals from a grateful local family physician or primary care provider. Of course, all the complaints would be for non-emergent issues that could wait until the morning.
But instead, after residency I took an employed position with a large HMO with great benefits. And all of a sudden, whenever I took call I was overseeing the urologic care of over half a million patients at once.
Call is still the worst part of my job
Unfortunately, I still hate the attending version of call that I have now. One of the main reasons I hate call is the uncertainty. It might be a tolerable night, or it might be an exhausting night full of back to back consults and surgeries. When I’m on call, my blood pressure jumps whenever I get a call or text message on my cell phone. We transitioned from pagers to iPhones, so when I’m on call, my cell phone is how the hospital reaches me. So that innocent text might be a message from my wife, or it also might be an emergency physician with bad news or CT scan findings that are going to ruin my night.
I also hate how I feel the next day.
If the gods are being merciful, I might be fairly functional the day after call. But if I have a bad call night, it rocks my world. Usually, I need about three days to recover before I feel normal again.
If by some miracle I get to sleep through the night without a call, I’m still tired the next day. This phenomenon was nicely summarized by Daniel Waters, DO, a retired cardiothoracic surgeon, in a Doximity Op-Ed: “You don’t sleep the same when you’re on call… Even after many years, you never learn to fully relax.”
It’s like sleeping with one eye open.
What do other physicians think?
When you Google around to find out which specialists hate their call the most, there’s surprisingly very little written about this topic. I’m fairly certain that most doctors hate call, but I didn’t have evidence of this. So I was very interested to see this following chain of events:
Doximity recently shared an article from KevinMD called “Stop dreading call.” It was written by Karen Leitner, MD, an internal medicine-pediatrics physician and life coach. In the article, she remembered the dread of overnight call. She recommended some mindset tips to use to stave off the negative feelings associated with call. Specifically, she recommended replacing negative thoughts with positive ones. It’s a common coaching tool.
Doximity boasts a community of over a million physicians. Because of this reach, I feel that it’s one of the best ways to take the pulse of the medical community in the United States. (They also have great taste and have shared a number of my posts.)
When I read through the comments, they were overall pretty scathing. Specifically, there were about 100 comments, and the vast majority disagreed with the post or spoke negatively about call. I went through all the comments and categorized them on a spreadsheet. Here’s the breakdown:
- 75% of the comments were negative with regards to overnight call.
- 14% of the comments were positive
- 11% were neutral or unrelated chatter.
Here is a graphical representation of my findings:
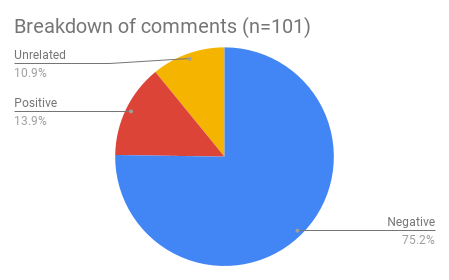
When I broke down the negative, positive, and unrelated comments by specialty, this is what I found:
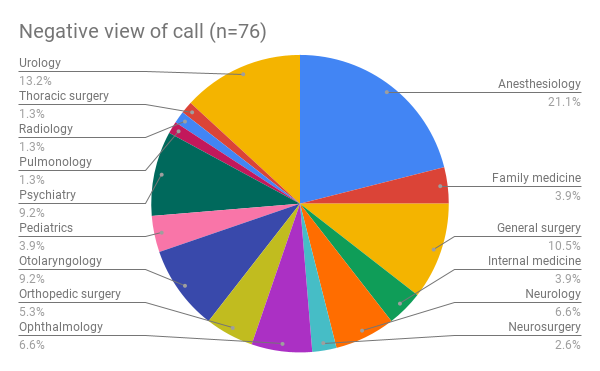
As you can see, I found that there are about 5 types of doctors that hate call. Anesthesiology, urology, and general surgery wrote the most number of negative comments about call. Together, they provided about 45% of the negative comments about call.
Psychiatry and otolaryngology rounded out the top 5 with 9% of the negative comments each. An honorable mention goes to neurology, with almost 7% of the negativity.
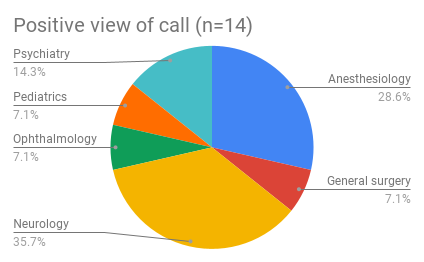
When it comes to positive comments about call, neurology, anesthesia, and psychiatry had the most.
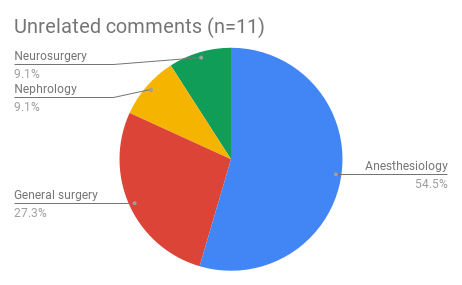
Anesthesiology and general surgery wrote the most unrelated comments.
Conclusions from the Doximity comments
I’ve come to the following conclusions from this data:
- General surgeons and urologists are unhappy about call
- Anesthesiologists mostly hate call but are more mixed — some hate it and some don’t mind it.
- Anesthesiologists like to post comments on Doximity.
Note: I absolutely know there are a lot of problems with this data. It’s not representative of all physicians. Also, there are a lot of variables to consider. Why did some specialists leave comments, while others did not?
Relationship of call to burnout
I found this data interesting, and wondered if this had any relationship to data on physician burnout, which is by many measures an epidemic amongst our nation’s physicians.
In a recent update to their annual surveys, Medscape published their 2021 burnout survey results. Here is the slide that shows the percent of specialists that reported being burnt out:
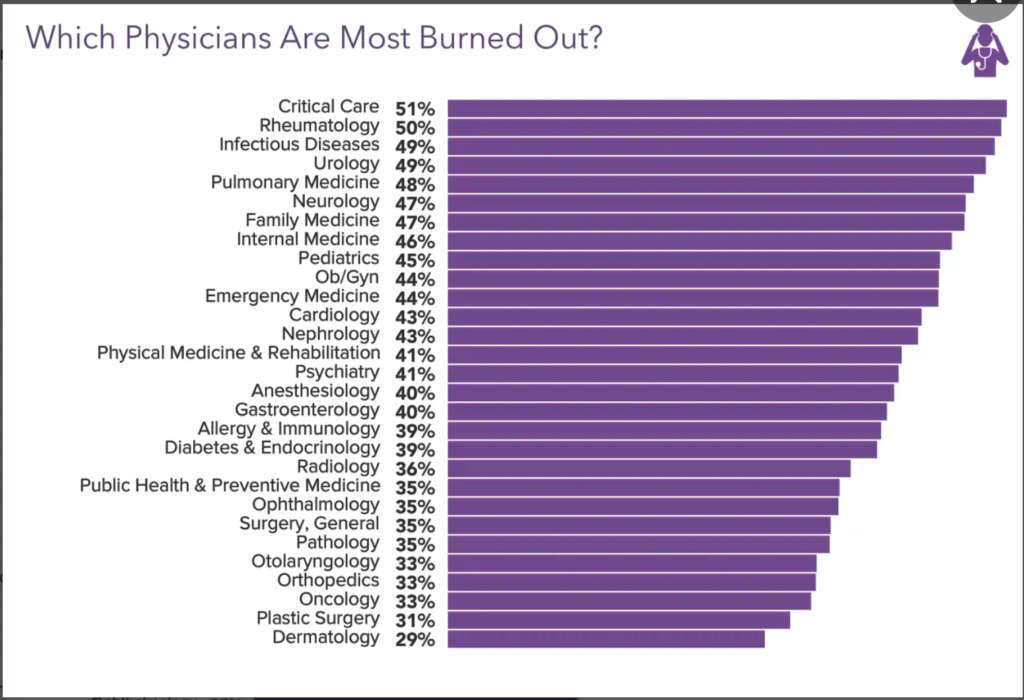
This is showing the effect of the Covid pandemic, with critical care, infectious disease, and pulmonary medicine taking top spots. These are specialists that have been on the front line of Covid since the pandemic began.
But while there were 5 types of doctors that reported hating call in the Doximity comments, not all of them seem to report high levels of burnout. When I combine this graph with the Doximity comments, the only specialties that report > 40% burnout and had >5% of the negative comments about call are:
- Urology
- Anesthesiology
- Psychiatry
Remember, the top specialists from the Doximity comments that seemed to hate call were: general surgery, anesthesiology, urology, psychiatry, and otolaryngology.
Honestly, I expected a better correlation between negativity about call to burnout rates. I think this demonstrates that medical specialties are very different. There are many factors why one specialty might feel burnt out in addition to unpleasant calls. For some it might be unpleasant overnight call, while for others it might be something about their day to day experience, like Covid patients.
But I was struck by the interesting finding that urologists seem to hate call and also report very high rates of burnout.
How to reduce burnout
Medscape also asked physicians about what needs to change for them to have less burnout.
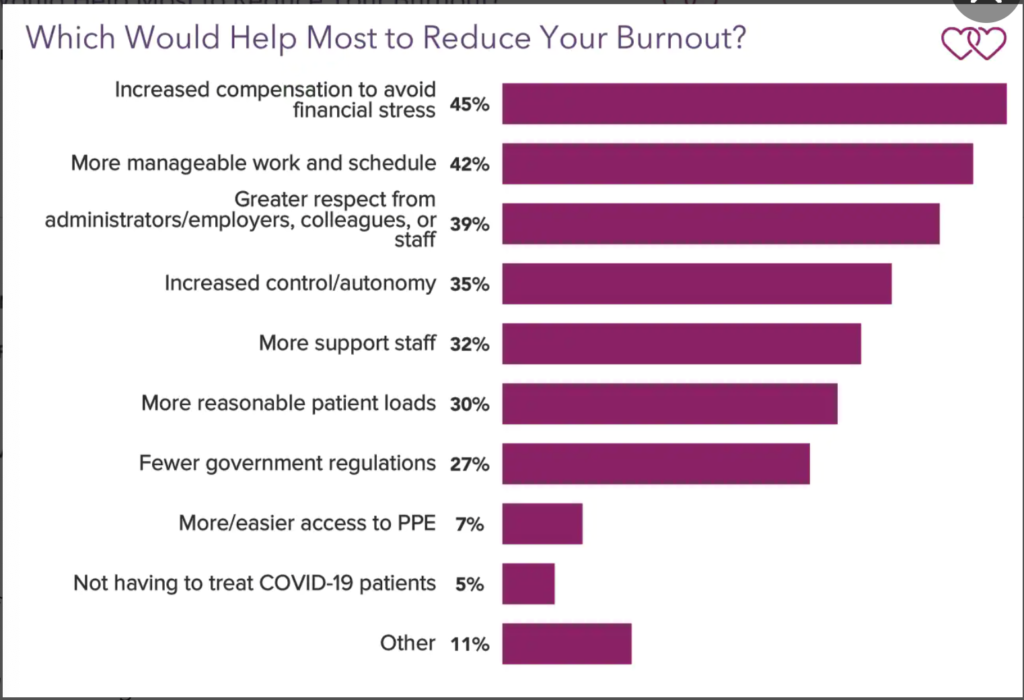
I’m not surprised by the finding that financial stress, work life imbalance, and lack of autonomy seem to be some of the top complaints of burnt out physicians.
moFIRE as a solution to burnout?
Longtime readers will know that I’m a big proponent of using index funds and real estate investing to achieve financial independence. I specifically am going for morbidly obese FIRE (moFIRE), which allows you to spend > $200,000 annually without traditional employment.
Three of the major reasons why I am striving for financial independence within the next 10 years is to have less financial stress, better work life balance, and more autonomy with my life. In fact, I started down this road to FIRE at a time in my life when I was feeling particularly burnt out.
Read more:
- My 15 year plan to financial independence, moFIRE style
- How rental cash flow cut 5 years off our plan to moFIRE
Conclusion
To summarize my findings, there are 5 types of doctors that seem to hate call: urologists, anesthesiologists, general surgeons, otolaryngologists, and psychiatrists. But only urologists manifest this hate with very high rates of burnout.
In any case, I am glad that there is more attention being placed on the the detrimental effects of physician call. While there are no good and easy solutions to this issue, the first step is to acknowledge that it’s an issue in the first place.
If we want there to be enough physicians to care for us in the future, we have to pay attention to things like this.
For as Dr. Waters stated in his Op Ed, “…call is what inevitably wears you down [sic]. … it is the submerged bulk of the iceberg that most people don’t see. The part that sinks ships.”
— TDD
Do you also hate call? Why is that the case? Please comment below and subscribe to my free weekly newsletter!
Are you a physician or physician spouse interested in using real estate to achieve financial independence?
Perhaps you’re more of a Facebook type?
Are you a physician, spouse, or professional and you’re interested in using Real Estate to gain financial freedom? Join us in our Facebook group and accelerate your journey!

Want to support the blog?
- Join our investor club at Cereus Real Estate
- Visit my Recommendations page
- Check out my wife’s food blog: Eat Dessert First
- Check out my TikTok channel
- Follow me on Instagram
- Follow me on YouTube
- Contact me with questions


Such a great post. I’m ENT and also hate call. Since it is considered home call it typically is not compensated or compensated lowly. When I was employed I was paid $200/night for my Q2 (!) call in a deferred comp model…none of which I ever received after 3 years. I was also charged PTO for Christmas (I was on call but “didn’t have scheduled clinic or OR” on a weekday). There is simply no acknowledgment from administration of the many negatives of call which you so clearly point out.
I am now in private practice and much happier. I do not take ER call (despite taking much sh*t from the local hospitals and employed ENT groups). I feel my “duty to my community” is accomplished by providing excellent care as a well rested early to mid career surgeon who gives every post op patient my cell phone number and am available without delay due to an unexpected face trauma consult. I also owe my young family the ability to be present on the weekends and evenings (although this is a continuous work in progress). I do pay for practice coverage when we travel (pre-pandemic we were hitting up 8-10 new countries a year most with our kids) but it cost significantly less than burning out so early in my career.
Your blog has been very helpful and I hope you keep up the excellent work.
Thanks for taking the time to write this! I’m sure your words will be very helpful to others who’d love to make a similar transition. I agree wholeheartedly that “home call” is a farce — it’s in many cases just as disruptive as just being in the hospital, with less appreciation from administration of this type of coverage.
It sounds like you made a well considered decision to have the practice that better fits with your lifestyle. How inspirational!
Amazing post! Fascinating review of the Doximity data.
Thanks Kirsten! My younger research oriented self from residency is groaning at the quality of the statistical analysis in this post, but whatever, it’s a blog, not a medical journal!
Great post! I’m a bit surprised that more physicians chose increased compensation over a more manageable schedule or better patient ratios to reduce burnout. Getting paid more is nice (especially while paying down loans) but a little less stress day to day seems like it would be more impactful
Thanks so much, Ashley! I think it’s hard to give up higher compensation, even when it becomes clear that the higher compensation comes at the expense of health, family, etc. I do certainly agree that a less stressful schedule is better for career longevity. It’s also harder to dial compensation if the lifestyle and spending has increased to match that higher compensation. I see this playing out in my own life soon, as I’d love to cut back a bit, but have to come to grips with the income change that will cause.
What happened to OB? I promise we hate call too!
Yes I’ve heard this! We decided on Facebook that the OBs were too busy on call to comment on Doximity, thus didn’t make the list.
I learned some new information today from this blog. That is indeed a good analysis. I’m sure your words will greatly help others wishing to make a similar transition. I wholeheartedly agree that “home visits” are bogus – in many cases, as disturbing as a regular hospital stay, with little appreciation of the administration of this type of coverage. It sounds like you made a well-considered decision to have practice more aligned with your lifestyle. Thanks for discussing this Amazing topic!
You’re quite welcome! Thanks for reading!
Hi! I’m a midwifery student and absolutely hate being on call. I’m very much thinking of pursuing another profession because of the effect it has on my mental health.
Yes, being on call can be very tough on sleep (obviously) and also mental health. Is being on call essential for midwifery? Are there positions where you don’t have to do it?